Redefining Ratings: Elevating User Trust and Conversion in Car Insurance
Azki’s mission
Azki is a web-based insurance aggregation platform that serves over 2 million users, empowering them to make informed insurance decisions with ease and confidence.
By offering expert guidance and a user-centric platform, we simplify the insurance selection process to help users find the best options tailored to their needs.
Conversion Bottleneck in Insurance Comparison
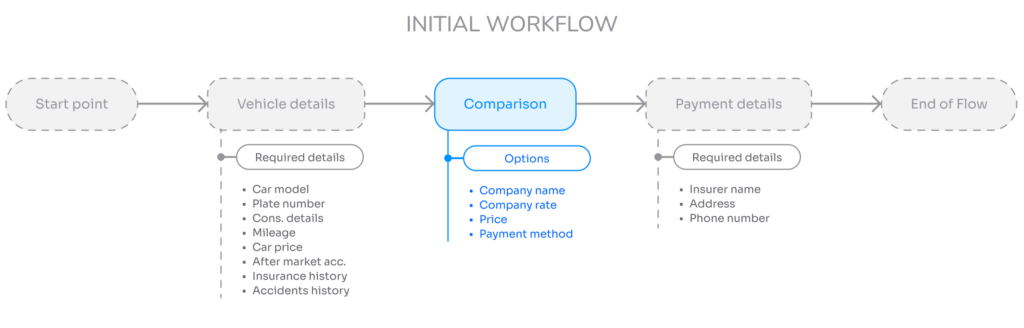
The car insurance funnel begins by requesting car details, followed by presenting a range of insurance options with varying prices, companies, and payment methods on the results page.
This stage experienced a high abandonment rate of 70%. While functional, it revealed significant pain points and challenges that needed to be addressed.
The Problem in Details
In addition to the low conversion rate, several other critical issues emerged:
📞 High Support Costs:
Over 35% of users contacted support to seek advice. Our support agents were restricted from recommending specific insurance companies, leading to increased operational costs without fully resolving user concerns.
😤 Customer Frustration:
Even after making a purchase, many users remained uncertain about whether they had selected the most suitable option, undermining their confidence in the platform.
⁉️ Misguided Decision-Making:
Users interpreted price differences as indicators of variations in service quality. This misunderstanding contributed to confusion and drop-offs as users struggled to make informed decisions.
🔥Impact
Number of support calls to ask for consultant decreased by 13%.
Conversion rate boosted by 2%.
We created the first platform for reviewing insurance companies’ services based on customer experiences.
My Role
I led research efforts, including qualitative interviews, user feedback collection, usability testing, and surveys. I also facilitated brainstorming sessions and design sprints, proposed solutions and evaluated their feasibility. And designed a high fidelity responsive page as the final solution.
🤝 In collaboration with:
- Junior product designer who assisted with user testing and research.
- The product manager who enabled workshops, testing, and feasibility studies.
- Development team, along with the technical manager, for technical feasibility and implementation aligned with the roadmap.
- A data analyst for data collection and analysis.
A Closer Look at the Design Process

Understanding Users
Analyzing quantitative data and historical user behavior for each segment revealed that users who struggle with price differences were often first-time buyers or those transitioning from offline to online purchases.
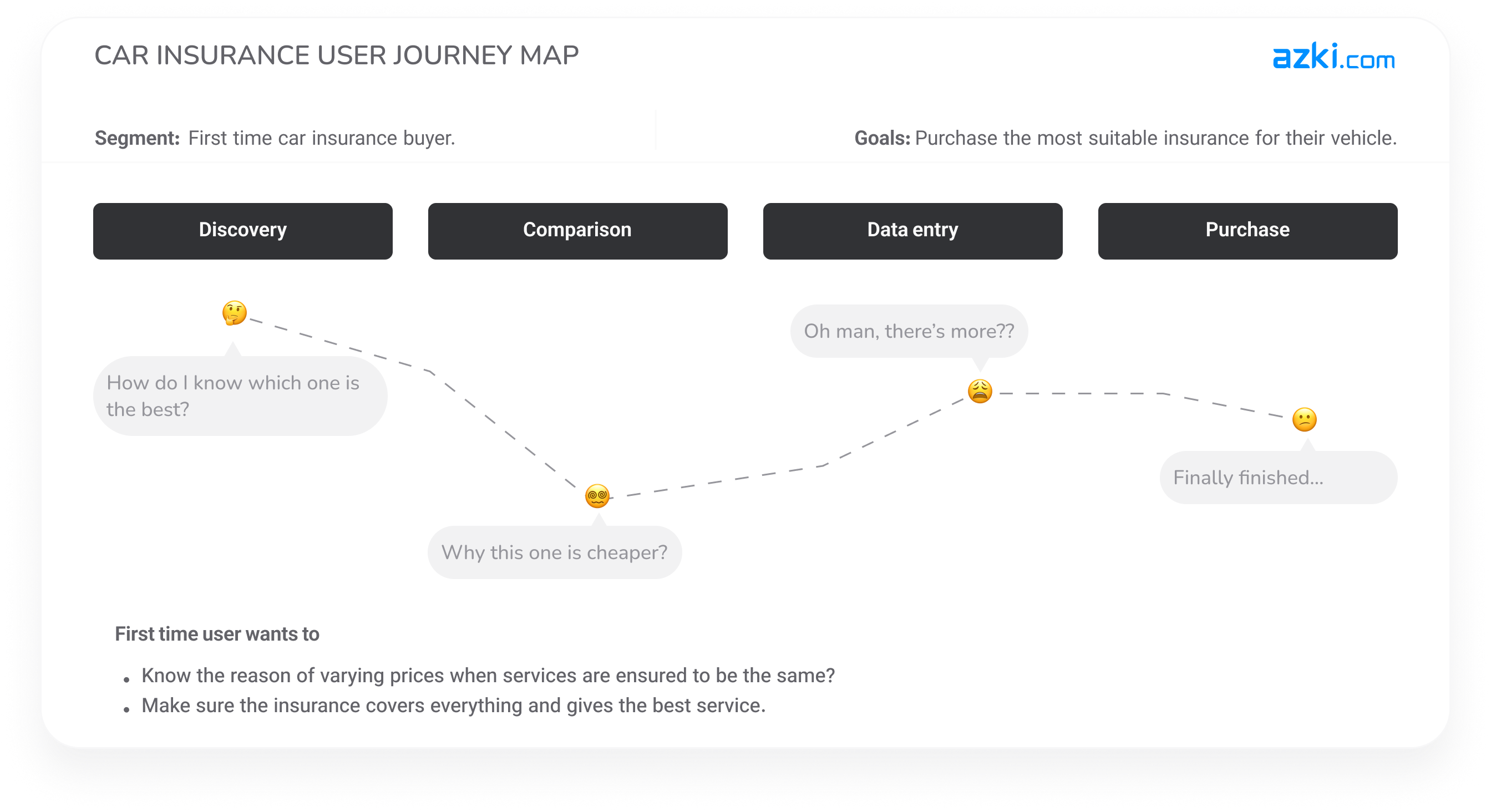
By collecting user feedback through different channels and cross-referencing it with historical metrics, We identified that almost all users struggled with price disparities and were unsure of which insurance suited their needs.
We also conducted user interviews combined with usability testing on users actively looking to purchase insurance.

🔎 Key Insights:
- Lack of Decision Clarity: Users found it challenging to decide which insurance was best for them.
- Experience-based Preferences: Many paused their purchase relying on ratings as a guidance.
- Unhelpful Support Responses: Some contacted online support, only to receive generic responses like “all companies provide similar services,” which contradicted the visible price variations.

Investigating Root Causes
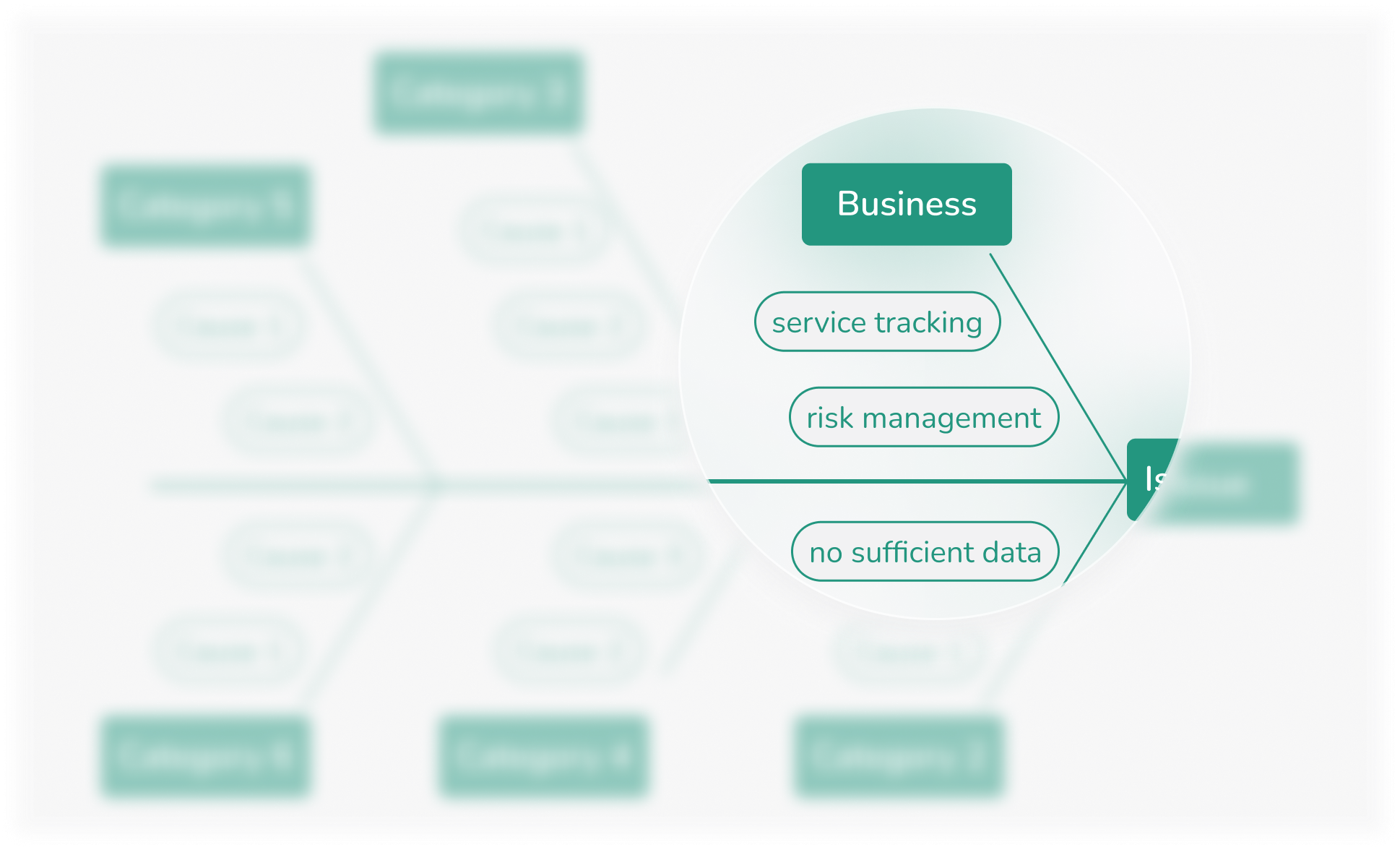
To identify the root causes, I asked key stakeholders from various departments to share their perspectives on the issue using the fishbone analysis technique.
🔎 Key Insights:
- The price differences stemmed from each company’s unique risk management policies. For instance, some considered newer car models low-risk, while others considered accident history a key role.
- The primary issue was insufficient user information about company services, such as claim processing times, customer support quality, and service reliability.
These workshops not only generated actionable insights but also fostered a culture of large-scale brainstorming within the organization.
These discussions clarified that creating an effective comparison tool would require addressing diverse risk management policies and integrating service quality metrics.

Solution to the root cause
The solution to enable users to compare options based on all contributing factors.
The primary issue was the lack of details to help users compare companies effectively, such as claim processing times, customer support quality, and service reliability.
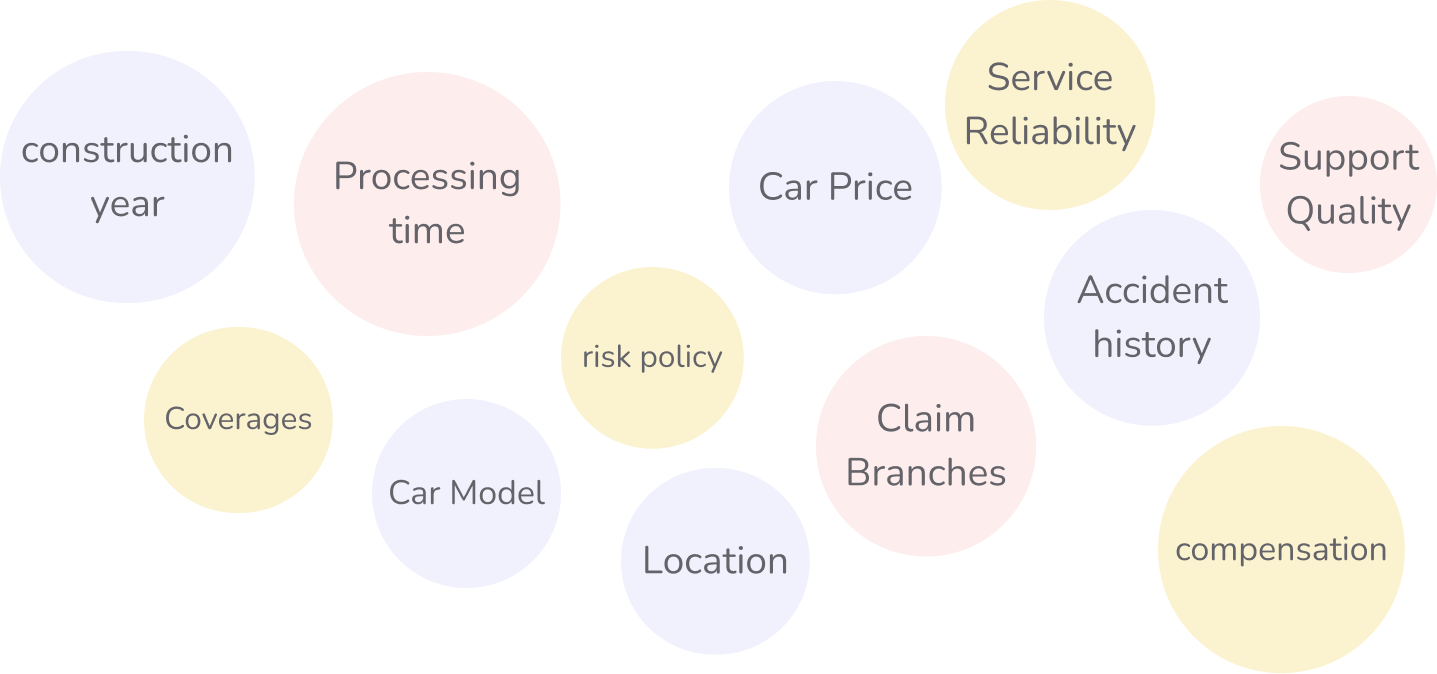
To address this, we needed a solution that would simplify the decision-making process while managing the complexity of collecting such diverse data.
The challenge was to create a system that could handle the variations in services across multiple companies, regions, and vehicle types.
We leveraged customer experiences as a scalable way to provide valuable insights into service quality.
By building on our existing rating system, we redesigned it to focus on key service aspects like claim handling and responsiveness. This allowed users to make informed comparisons quickly and confidently.
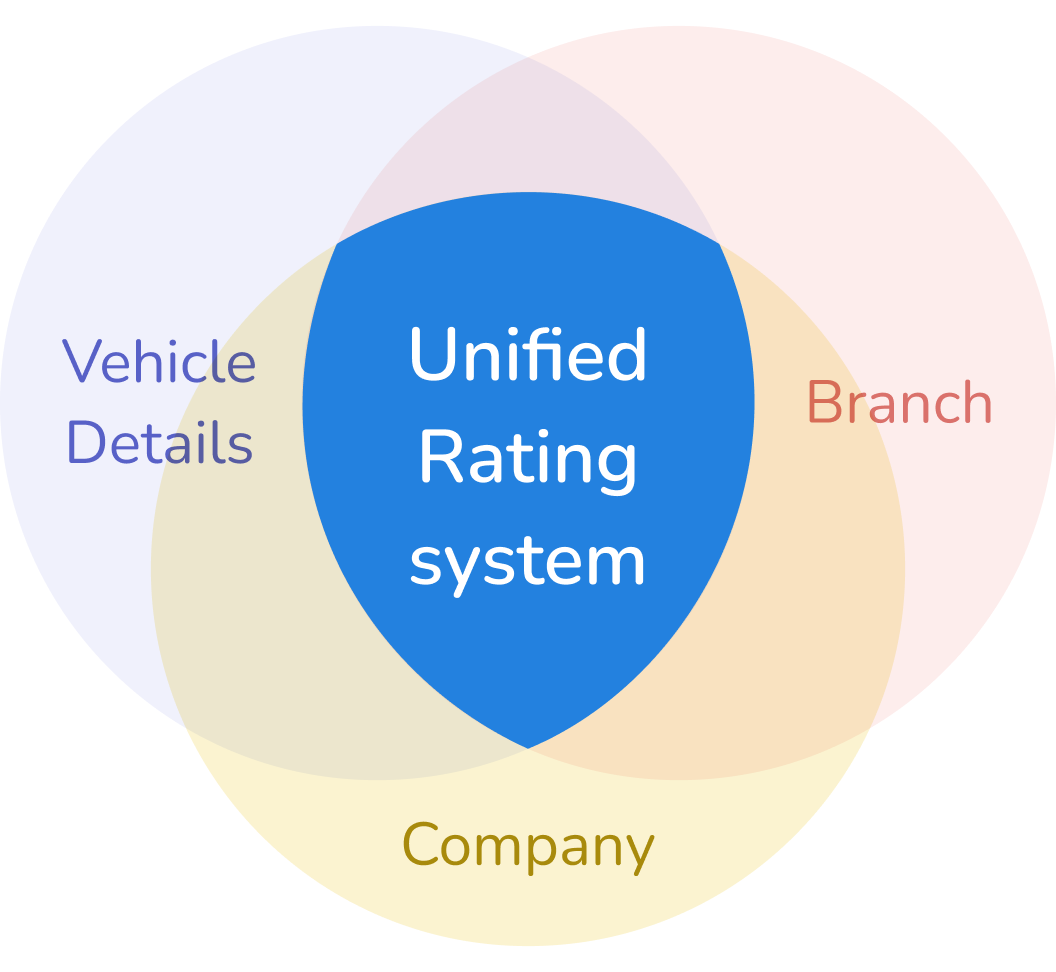
The solution was not only cost-effective but also embraced by stakeholders for its simplicity and impact, reinforcing Azki’s role as a trusted guide in insurance selection.
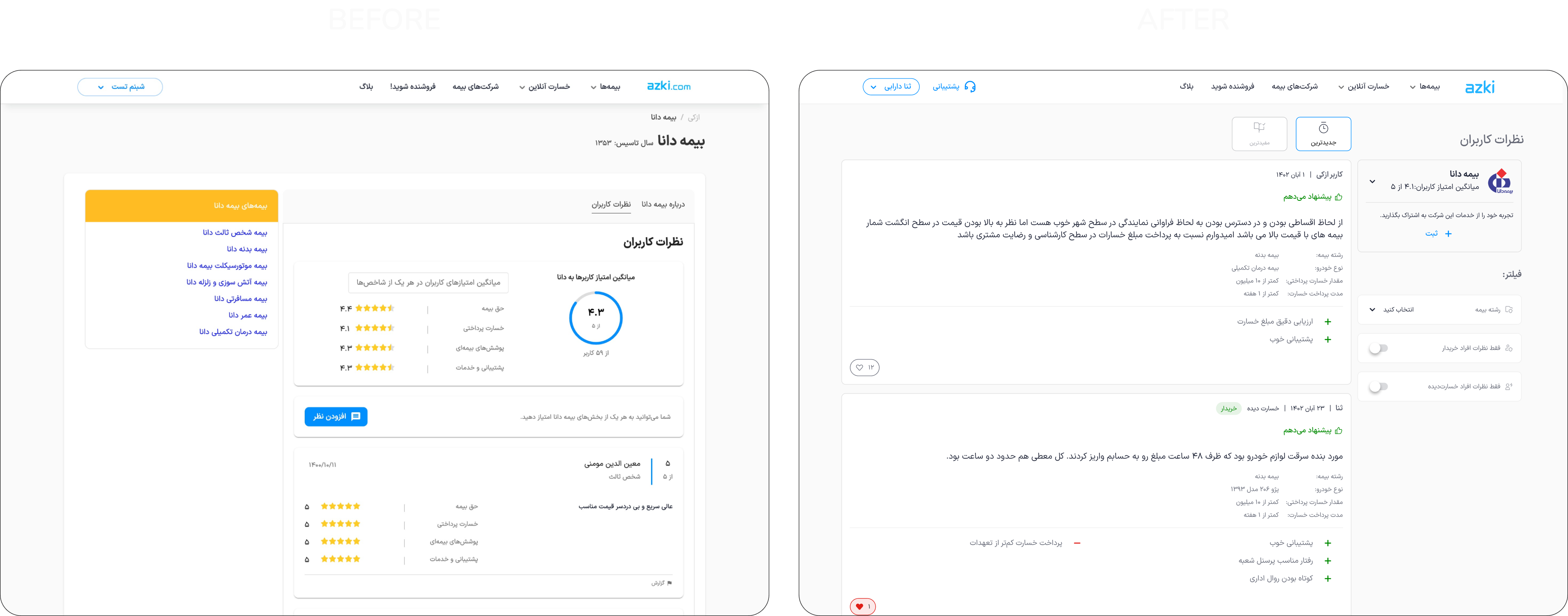
We redesigned the rating and review feature with the aim of collecting validated, unbiased user experiences to compare services across companies.

The outcome was revamping Rate And Review system in Azki.
The final design offered two clear paths: proceed with inspection for new coverage or skip it by continuing previous conditions.

solution success metrics
We decided to proceed with the solution for several reasons.
- There was unanimous agreement among key stakeholders, including the CEO and CPO, that it had the potential for a significant impact.
- The nature of the solution required at least four months to show measurable results.
To ensure we could track its progress effectively, we established clear success metrics to monitor performance and identify any deviations early on
🏆 Success metrics
- Increase Result Page Conversion: Measuring how many users complete their purchases after using the enhanced comparison tool.
- Decrease Number of Users Seeking Consult: Tracking a reduction in support inquiries related to decision-making, indicating that users find the comparison tool helpful.
💡 Health metrics
- Increase Useful Comments: Ensuring that the quality of user feedback remains high and relevant to guide informed decisions.
- Increase The Directory of Comments: Monitoring the growth of reviews in the directory to validate consistent user engagement.

Final Design release
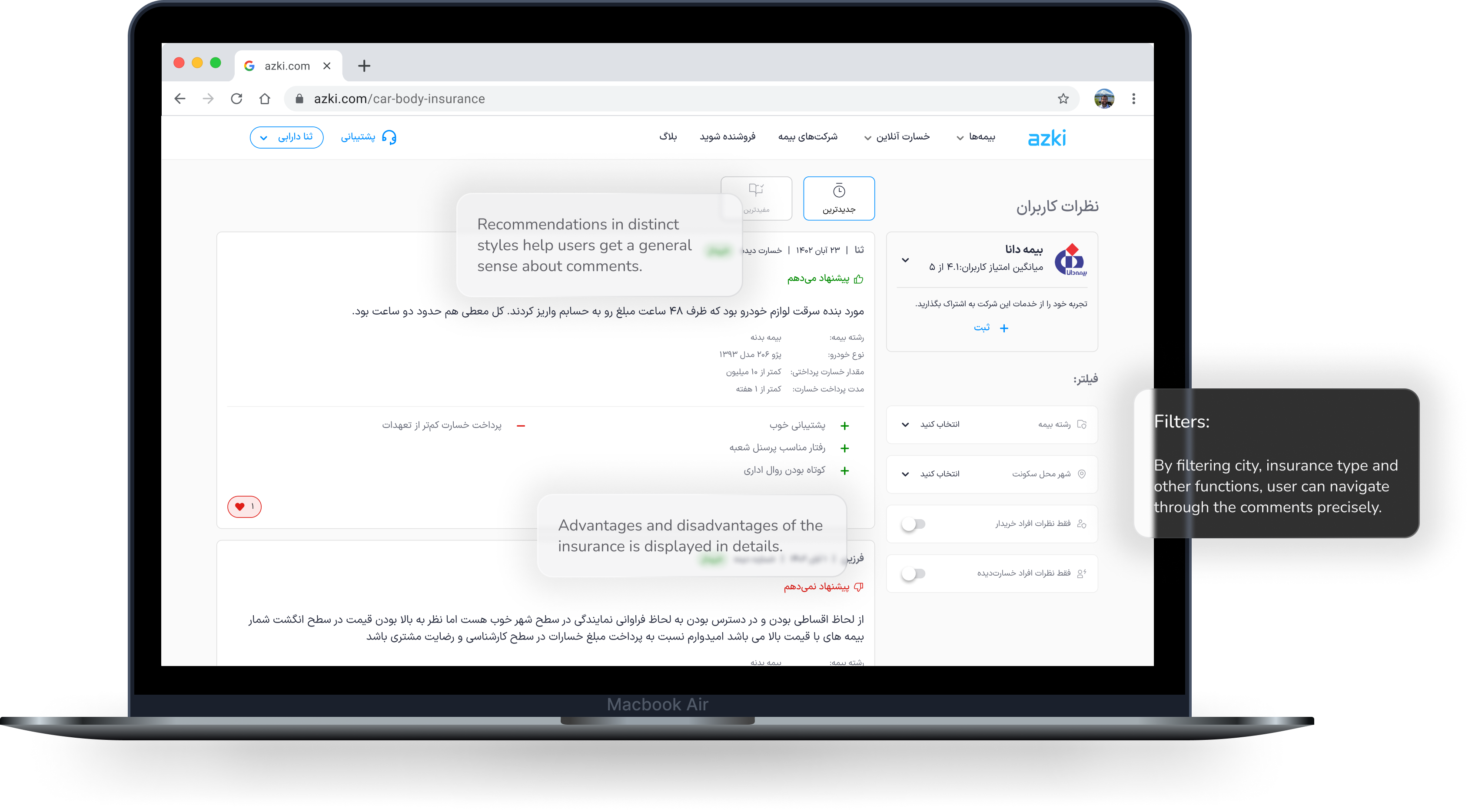
The final solution included various aspects, including the “leave a comment flow” and “rating reflections.” However, the Comments Page served as the central touchpoint, enabling users to gain a comprehensive understanding.
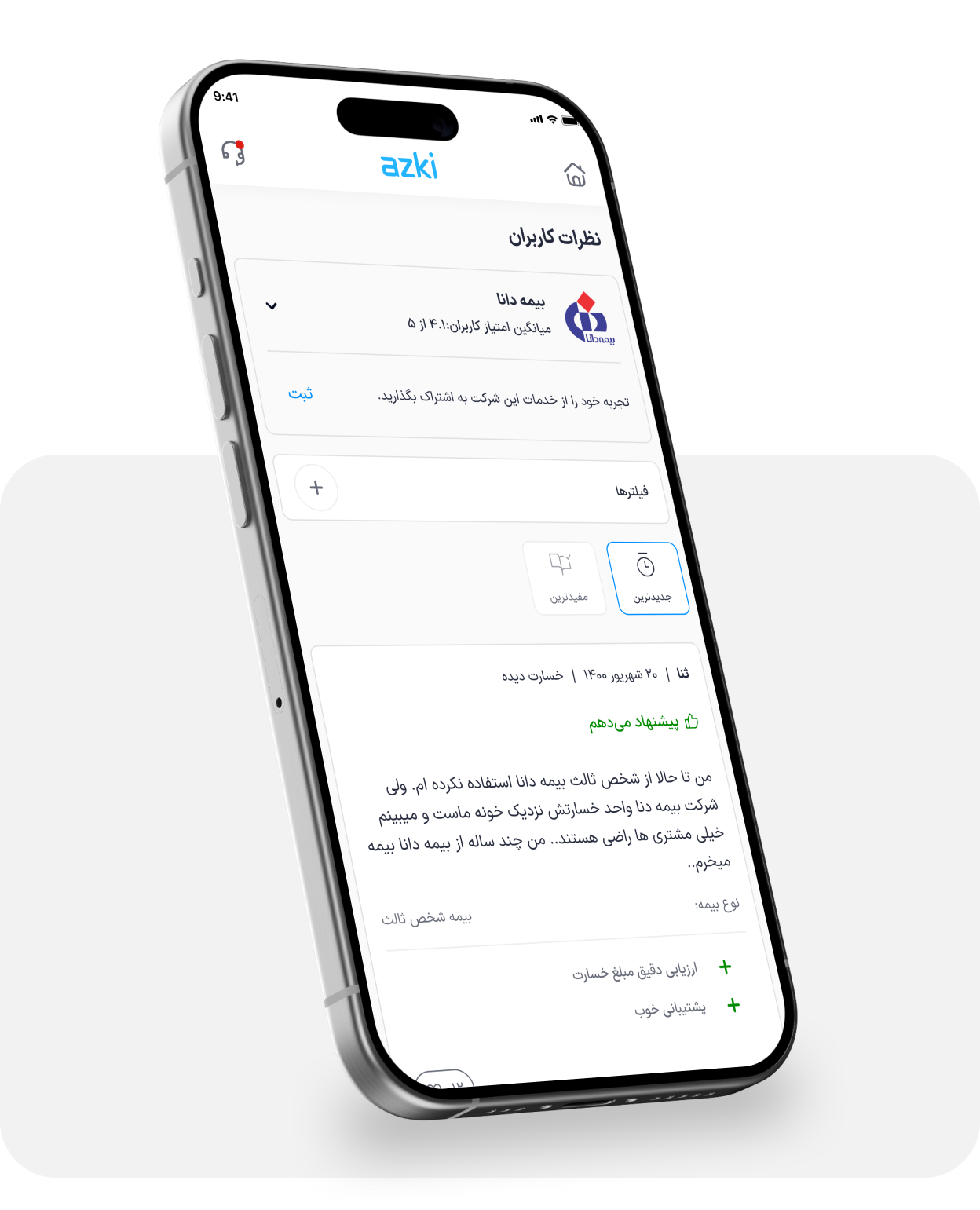
🎯 Future Plans
My goal is to leverage user reviews about insurance companies and their services to recommend the most suitable insurance based on users’ needs which aligns with Azki’s mission.
The next step would involve utilizing AI to analyze the services of each company based on user conditions and provide personalized insurance recommendations to users.
Results
✍️ 60% increase in useful reviews, which significantly improved the review directory’s utility.
💪 Within 6 months, we gathered numerous reviews highlighting poor staff behavior at a top-selling insurance company. Azki leveraged this feedback to persuade the company to improve its customer interaction protocols, boosting customer satisfaction by 25%.
The feature significantly enhanced brand trust, establishing Azki as a comprehensive insurance comparison platform.
Reflections
In this project, I learned how to identify and raise awareness about a long-ignored problem and present compelling data to stakeholders, effectively persuading them of its importance.
Additionally, I honed my ability to facilitate brainstorming sessions with key stakeholders.
This collaborative approach not only enriched the final outcome but also fostered alignment and shared ownership among the team.